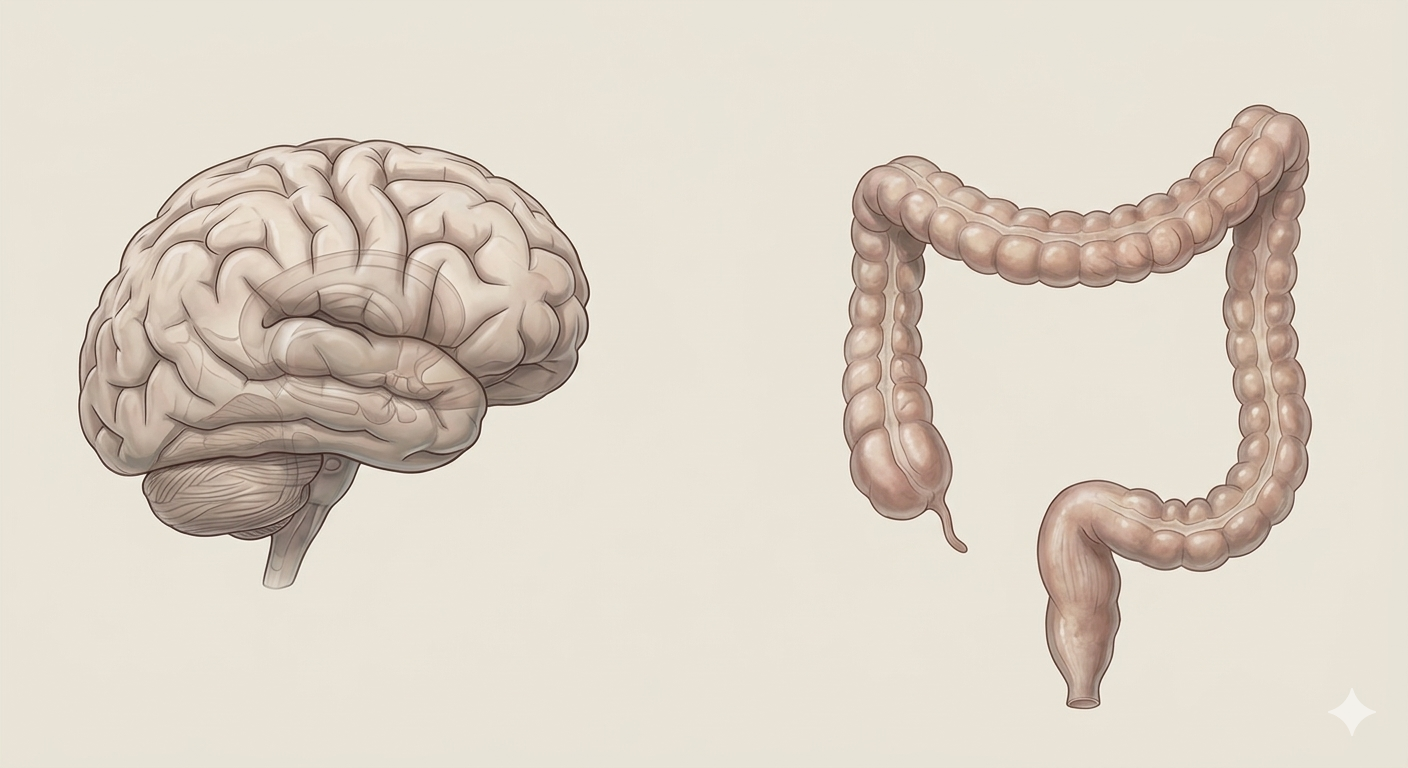
Ulcerative colitis (UC) is a long-term inflammatory disease that affects the large intestine, also called the colon. It causes symptoms such as abdominal pain, diarrhea, blood in the stool, fatigue, and weight loss. UC is one type of inflammatory bowel disease (IBD). While UC mainly affects the digestive system, research shows that it can also affect the brain and mental health. This connection occurs through a system known as the gut–brain connection, or gut–brain axis.
The gut–brain axis is a two-way communication system between the digestive system and the brain. It allows the gut and brain to send signals to each other using nerves, hormones, immune responses, and gut bacteria. One of the key parts of this system is the vagus nerve, which directly links the brain to the digestive tract. When the gut is healthy, this communication helps regulate digestion, mood, and stress. However, when the gut is inflamed for long periods, as in ulcerative colitis, this communication can become disrupted and may affect brain function (Carabotti et al., 2021).
Inflammation plays a major role in how UC affects the brain. During flare-ups, the immune system releases chemicals called cytokines. Cytokines help the body respond to inflammation, but high levels can be harmful. Some cytokines enter the bloodstream and reach the brain. Once there, they may affect areas of the brain that control mood, sleep, memory, and stress responses (Encyclopedia MDPI, 2021). This may explain why people with UC often experience fatigue, anxiety, or emotional distress, even when bowel symptoms are mild.
Gut bacteria are another important part of the gut–brain connection. The gut contains trillions of bacteria that help digest food, support the immune system, and produce substances that protect the gut lining. Some of these substances, such as short-chain fatty acids, also support brain health and help reduce inflammation. In people with UC, the balance of gut bacteria is often disturbed. This imbalance is known as dysbiosis. Dysbiosis can increase inflammation and send harmful signals to the brain, which may negatively affect mood and thinking (Carabotti et al., 2021).
Mental health conditions are more common in people with ulcerative colitis than in the general population. Anxiety and depression are the most reported concerns. Studies show that about one-third of people with UC experience anxiety or depression at some point during their illness (Medical News Today, 2023).
Although living with a chronic illness can be stressful, research suggests that mental health symptoms in UC are not caused by stress alone. Instead, changes in inflammation, immune activity, and gut bacteria can directly influence the brain through the gut–brain axis.
Brain imaging studies provide further evidence of this connection. Magnetic resonance imaging (MRI) studies have found differences in brain structure and activity in people with UC compared to those without the disease. Some changes appear in areas of the brain involved in emotional regulation, pain processing, and decision-making. These changes are associated with higher levels of anxiety and depression and are more noticeable in people who have had UC for a longer time (Mandl et al., 2021). This suggests that ongoing inflammation in the gut may gradually affect the brain.
Functional brain studies also show that people with UC may respond differently to stress. Areas of the brain such as the amygdala, which helps process fear and emotions, may become more sensitive. This sensitivity can lead to a cycle where stress worsens gut symptoms, and worsening gut symptoms increase emotional distress. Because the gut and brain constantly communicate, problems in one system can strongly affect the other.
Understanding the gut–brain connection is important for the treatment of ulcerative colitis. UC care should not focus only on managing bowel symptoms. Mental health screening should be included as part of routine care. Early identification of anxiety, depression, and stress can help improve overall well-being and may reduce symptom flare-ups. Supportive treatments such as counseling, stress management, relaxation techniques, and patient education can help people better manage their condition.
There is also increasing interest in treatments that focus on improving gut health. Dietary changes, probiotics, and medications that reduce inflammation may help restore balance in the gut. Improving gut health may also improve mental health by reducing harmful signals sent to the brain. Although more research is needed, these approaches support the idea that ulcerative colitis should be treated using a whole-person approach.
In conclusion, ulcerative colitis is not only a disease of the digestive system. Through the gut–brain connection, UC can also affect brain function, mood, and mental health. Chronic inflammation, immune system activity, and changes in gut bacteria all play a role in this process. Understanding the relationship between the gut and the brain allows healthcare providers to offer more complete care. By addressing both physical symptoms and mental health needs, people living with ulcerative colitis may achieve better health outcomes and an improved quality of life.
References
Carabotti, M., Scirocco, A., Maselli, M. A., & Severi, C. (2021). The gut–brain axis:
Interactions between enteric microbiota, central and enteric nervous systems.
International Journal of Molecular Sciences, 22(16), 8870.
Encyclopedia MDPI. (2021). Gut–brain axis in inflammatory bowel disease.
Medical News Today. (2023). Ulcerative colitis and mental health.
Mandl, T., et al. (2021). Altered brain connectivity in patients with inflammatory bowel
disease. Neurogastroenterology & Motility.